PC3I’s Cancer Care @ Home “Tackles a New Frontier”
February 4, 2021
In 2020, Penn Medicine delivered cancer treatments to nearly 1500 patients in the comfort of their own homes. While a few national providers have recently announced they will invest in the trend, no other providers in the region have made this transition from hospital or outpatient treatment to home, according to a recent Philadelphia Inquirer article. The article explores why Penn is so far ahead of the nation in the new frontier of at-home cancer care delivery, noting PC3I’s Cancer Care @ Home (CC@H) program as the driver of Penn’s successful innovation.
Building on international research demonstrating the safety of delivering certain cancer treatments to appropriate patient populations at home, PC3I launched the CC@H demonstration program in February 2020, referring 39 patients with breast cancer, prostate cancer, and lymphoma in its first month. The launch of the program soon accelerated when patients and providers sought other options for their treatment, hoping to reduce non-essential hospital visits due to COVID-19. At its core, the program strives to be patient-centric, fitting into patient schedules and empowering them to go about their days and spend time at home with their families instead of in the hospital or clinic.

Providing cancer treatment at home is not a new concept but has been looked at cautiously by many health providers wary of costs or fearful of change. Richard Snyder, chief medical officer for the parent company of Independence Blue Cross, noted, “Physicians and hospitals tend to be creatures of habit.” In fact, Penn’s program is the largest program of its kind in the United States. Snyder told the Inquirer that Penn is at the forefront of moving chemotherapy to the home.
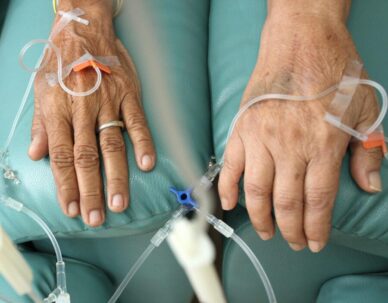
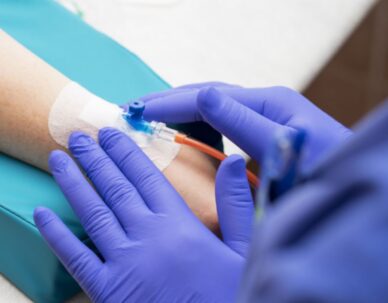
Among the nearly 1500 Penn patients who have received cancer care at home in the last year is Lisa Oney, 33, who is able to run errands and care for her children while carrying a backpack that delivers chemotherapy intravenously. Oney was diagnosed with lymphoma in November and, after an initial round of chemo in the hospital to ensure there were no adverse reactions, is continuing her treatments at home.
While in-home infusions are significantly less costly for insurers, hospitals may experience a financial loss under the current payment model when making the transition to home administration of cancer drugs. Justin E. Bekelman, MD argues for a new payment model that offers “a crucial incentive for health systems to invest in providing more care at home and other less expensive locations—a shift that should ultimately save insurers money.”